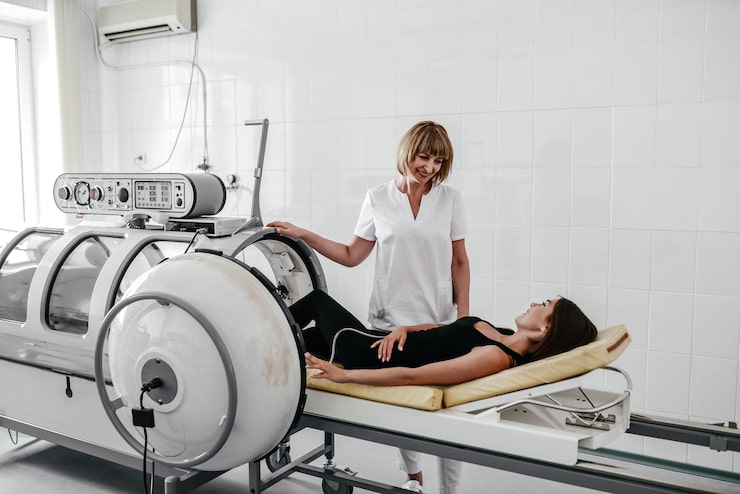
The HBOT Difference
At Prana, we believe oxygen is the foundation of true health-and Hyperbaric Oxygen Therapy (HBOT) is for everyone, not just elite/athletes/critical care patients. Whether you’re seeking faster recovery, sharper focus, enhanced energy, or long-term vitality, our science-backed approach helps you unlock your body’s full potential-one breath at a time.
expert therapist
advanced techniques
personalized care